Kontakt
CaviTAU®
Die bildgebende Ultraschallermittlung der Knochendichte und Knochenqualität im Kiefer
Die Funktionsweise
Die Funktionsweise von CaviTAU® bezieht sich auf das Erkennen und Lokalisieren von Kavitäten (= vermehrte Hohlräume bis zur fettig-degenerativen Auflösung der medullären Trabekelstrukturen) in Kieferknochen unter Verwendung der trans-alveolaren Ultrasonographie (Through Transmission Alveolar Ultrasonography, TAU).
CaviTAU® erzeugt einen Ultraschallpuls und leitet den Puls durch den Kieferknochen. Der Impuls wird anschließend von einer Ultraschallempfangseinheit erfasst und ermittelt. Abschwächungen der Amplitude des Pulses zeigen pathologische Veränderungen im Kieferknochen an. Die Ergebnisse werden auf einem Farbmonitor angezeigt und zeigen je nach Dämpfungsgrad unterschiedliche Farben.
CaviTAU® ist ein Messgerät zu einer röntgenstrahlenfreien Tiefendiagnostik durch den Zahnarzt
Diese Form der Ultraschalldarstellung der Kieferregionen erlaubt das Lokalisieren von möglichen Entzündungsbereichen im Kiefer mittels einer strahlungsfreien Befundung.
Untersuchungen, die mittels CaviTAU®-Geräten durchgeführt werden, helfen zur Auffindung jeglicher entzündlicher sowie degenerative Prozesse im Kiefer an, geben aussagekräftige Informationen zur Knochenqualität wieder und verhelfen zu forensischen sauberen Arbeiten.
Die zuverlässige Methode zur Bestimmung der Knochendichte vor Einsatz eines Zahnimplantats macht das CaviTAU® Sonographie-Gerät auch zu einem wertvollen Begleiter in der Implantologie. Es leistet einen wesentlichen Beitrag, präoperativ das Implantationsergebnisse von vornherein besser zu bestimmen.

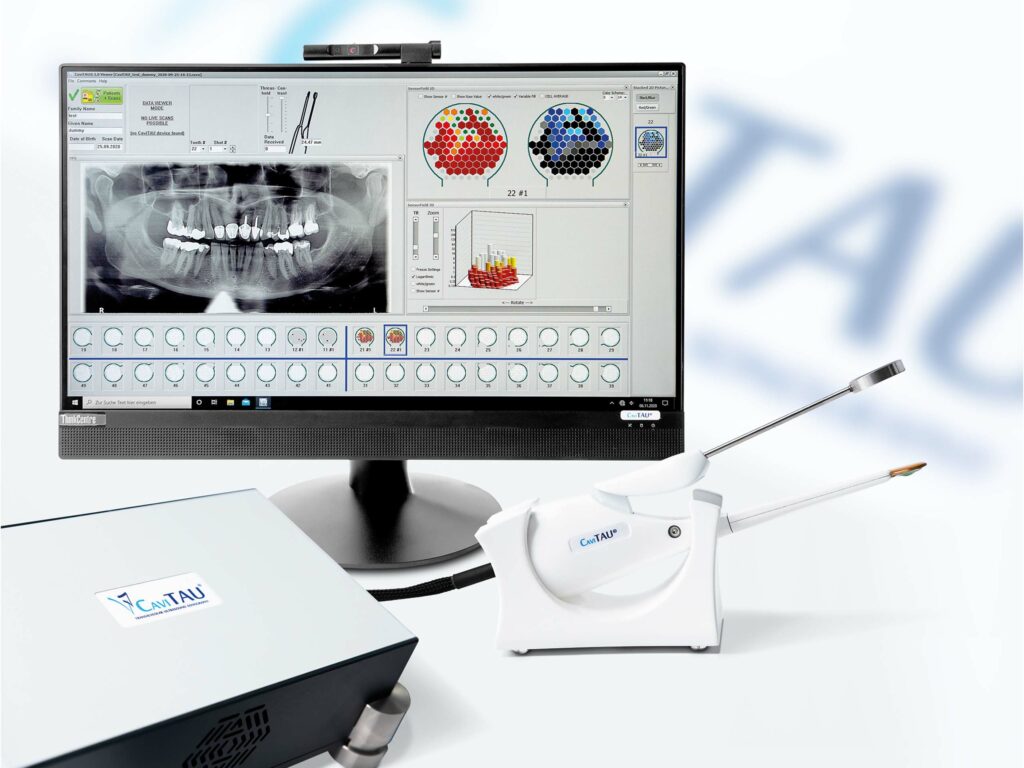
CaviTAU® ist ein weltweit einzigartiges Instrumentarium in der Dentalmedizin, die mit der Röntgentechnik immer wieder an ihre Grenzen stößt
Nicht ausgeheilte, alte Entzündungen, beispielsweise nach Zahnextraktionen, entwickeln sich nicht selten zu Entzündungsbereichen, welche sich immer wieder der Röntgenbefundung entziehen. Im Gegensatz zu den in der Medizin verwendeten Ultraschallgeräten – durchdringen die Schallwellen des CaviTAU®-Gerätes speziell das Weichgewebe (Wangen) und den Kieferknochen so, dass harter Knochen von weichen Knochen unterschieden werden kann.
So lassen sich sogenannte Kavitäten im Kieferknochen lokalisieren, von denen bekannt ist, wiederum sogenannte fettig-degenerative Osteonekrosen/Osteolysen (FDOKs) zu beheimaten.
CaviTAU® ist ein mit umfangreichem Datenmaterial aus Praxis und Labor belegtes und wissenschaftlich validiertes Verfahren. Zahlreiche wissenschaftliche Arbeiten belegen die Funktion und beschreiben darüber hinaus die CaviTAU®-Befundung als die präzisere Methode zur sicheren Lokalisation der FDOKs.
Das Medizinprodukt CaviTAU® ist ein System aus folgenden Komponenten.
- Basisgerät inkl. Fußschalter/Maus/Tastatur mit Funkanbindung
- Handstück inkl. Gelkissen
- Bildschirm/Software inkl. grafischer Nutzerschnittstelle (GUI)
- Verpackung sowie Kennzeichnung inkl. Nutzerdokumentation
Die Messeinheit für enorale Ultraschallmessungen umfasst einen Ultraschallsender und einen Ultraschallempfänger, (“Messeinheit”) in einer klar definierten, festen geometrischen Position zueinander.
In CaviTAU® wird die Messeinheit vorzugsweise Komplanarität positioniert. Um eine klar definierte, feste geometrische Position bereitzustellen, sind die beiden Teile der Messeinheit miteinander verbunden. Mindestens ein Arm ist drehbar, so dass die beiden Teile der Messeinheit einen Greifer bilden. Durch den Einsatz starrer Arme ist die Konstruktion der Messeinheit so stabil, dass eine durch mechanische Belastung verursachte Fehlfunktion des Empfängers praktisch ausgeschlossen ist.
Die Koplanarität von Sender und Empfänger ist ein wesentliches Merkmal der CaviTAU®-Konstruktion. Der Greifer wird leicht zusammengedrückt, wenn sich beide Teile der Messeinheit in der optimalen Position befinden, um eine akustische Leitfähigkeit zwischen der Messeinheit und dem Kieferknochen zu gewährleisten.

CaviTAU® ist ein unerlässliches Instrument zur Aufdeckung chronischer Entzündungen bei allen immunologischen Systemerkrankungen
Nicht nur die unerkannte blande Osteopathie des Kieferknochens in Form der fettig-osteolytischen-Osteonekrose kann zu einem systemischen Stressfaktor werden, sondern auch unverträgliche Materialien oder Medikamente führen häufig zu einem Entgleisen des Immunsystems und langfristig gesehen ebenfalls zur Entstehung von FDOKs. Somit lassen sich zahlreiche Immunerkrankungen durch die Befundung mit dem CaviTAU®-Gerät erklären oder Zusammenhänge aufdecken.

Sichere und einfache Handhabung
Mit dem neuen CaviTAU®-Gerät ist eine einfache Handhabung gewährleistet, die es ermöglicht, die Befundung in die Hände von Assistenz-Personal zu geben. Mittels gezielter Schulungen und Trainings sind die CaviTAU®-Ärzte in der Lage, in wenigen Trainingseinheiten die sichere Anwendung des Gerätes zu erlernen und die Interpretation der Auswertung anzuwenden.

Genaue und aussagekräftige Ergebnisse
Mit dem neuen CaviTAU®-Gerät – wurde höchste Priorität auf die Empfindlichkeit der Apparatur und des verwendeten Auswertungsverfahrens gelegt. Durch eine neue, innovative Konstruktion der Messeinheit und durch neue Wege zur Gewährleistung einer guten akustischen Leitfähigkeit zwischen dem Kieferknochen des Patienten und der Vorrichtung – werden präzise und aussagekräftige Ergebnisse erzielt, die den Arzt in die Lage versetzen, seine Diagnostik darauf aufzubauen.


